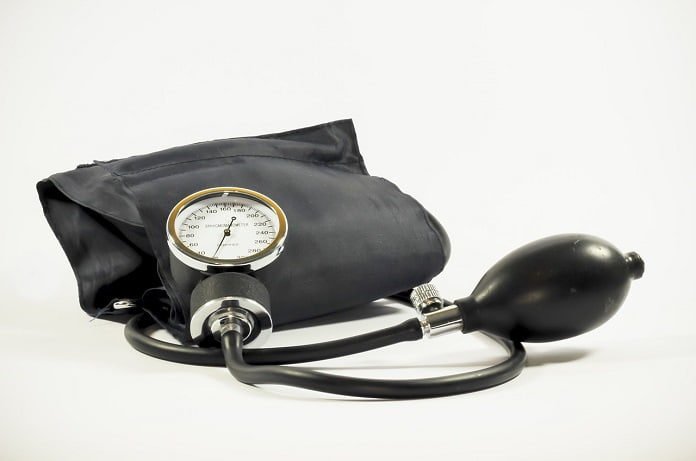
Researchers investigated how blood pressure monitoring by individuals affects blood pressure control and whether it benefits particular patient groups.
The article below contains sponsored links to other sites; these links are being provided as a convenience and for informational purposes. The editorial staff of the Medical News Bulletin had no role in the preparation of the contents of these linked sites and are not responsible for the accuracy or content of the linked sites. The views and opinions expressed in the sponsored links are those of the advertiser and do not reflect those of the Medical News Bulletin. The Medical News Bulletin does not accept liability for any loss or damages caused by the use of any products or services, nor do we endorse any products, services, or links in our sponsored links.
Patients with hypertension (high blood pressure) who are self-monitoring blood pressure in addition to the usual anti-hypertensive treatments and care appear to have better blood pressure control than those who are not.
However, the use of blood pressure monitoring by individuals is inconsistent and its effects are not well understood.
Researchers at Oxford University, in the UK, wanted to better understand the effects of self-monitoring blood pressure. In particular, they looked at the interaction of blood pressure monitoring by individuals with other supportive interventions in hypertension – such as lifestyle counseling or support from a health professional.
They also examined whether the benefits of self-monitoring vary between patient subgroups – such as gender, different number of medications, or patients with coexisting conditions, such as diabetes or obesity.
They recently reported the findings of their study in the journal PLoS Medicine.
The researchers performed a systematic search of the published medical literature to find all studies that examined blood pressure monitoring by individuals with hypertension.
From these, they selected studies since 2000 with at least 100 patients and a six-month follow-up period.
They contacted the authors and asked for access to the original data collected for each patient.
They obtained data from 15 out of 19 studies (7,138 out of 8,292 patients) and used this in a new combined analysis to evaluate the effect of self-monitoring on blood pressure levels and the control of hypertension after one year of follow-up.
They looked at whether any additional supportive interventions had been used and graded these from Level 1 (no support) to Level 4 (support from a medical professional throughout the trial).
In addition, they looked at outcomes in different patient subgroups – gender, age, blood pressure level at the start of the study, number of medications at the start of the study, history of heart attack or stroke, and coexisting conditions such as diabetes, kidney disease, or obesity.
Overall, at 12 months follow-up, self-monitoring was associated with reduced blood pressure compared to usual anti-hypertensive care. However, this effect was strongly influenced by the intensity of other supportive interventions, ranging from no effect with self-monitoring alone, to a 6.1 mmHg blood pressure reduction when monitoring was combined with intensive support (Level 4).
Intensive support could include systematic medication dose adjustment by doctors or other medical staff, health education, or lifestyle counseling.
Looking at various subgroups of patients, blood pressure monitoring by individuals was most effective in those with fewer antihypertensive medications and those with higher blood pressure at the start of the study.
No differences in efficacy were seen in subgroups according to gender or by most co-existing illnesses.
The researchers concluded that self-monitoring, by itself, is not associated with lower blood pressure or better control. However, when combined with other supportive interventions, self-monitoring leads to clinically significant blood pressure reduction and this continues for at least 12 months.
Self-monitoring can be recommended to lower blood pressure when combined with such interventions, which involve tailored individual support.
Self-monitoring may also be useful for other reasons, such as engaging with patients or helping to reduce doctors’ workload.
Written by Julie McShane, Medical Writer
Relevant topics that may be of interest to you:
- Can a natural substance from spirulina lower high blood pressure?
- Regular use of sleeping pills may increase the use of blood pressure medication
- Can a plant-based diet affect blood pressure?
- What Should Your Blood Pressure Target Be?
- Controlling blood pressure in older individuals may increase mortality rates
- A New and Improved Sunscreen with an Old Blood Pressure Drug?
- Can Magnesium Help Lower Blood Pressure?
Reference: Tucker KL, Sheppard JP, Stevens R, et al. (2017) Self-monitoring of blood pressure in hypertension: A systematic review and individual patient data meta-analysis. PLoS Med 14(9):e1002389. https://doi.org/10.1371/journal.pmed.1002389.