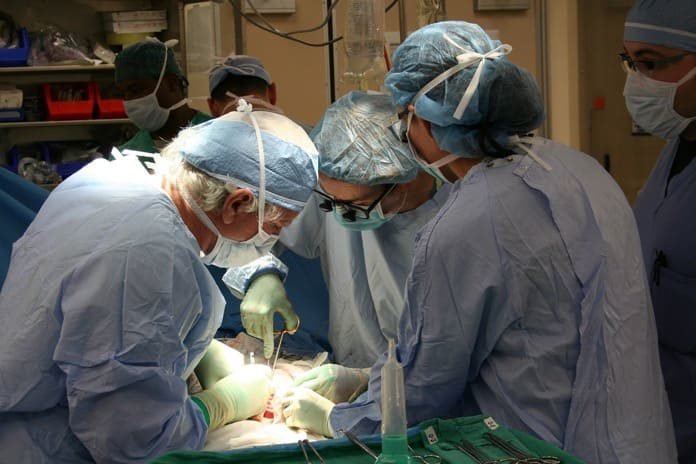
Researchers compared post-operative weight gain in patients who had undergone liver transplant alone with those who had a weight loss surgery at the same time.
Liver transplants in obese patients with fatty deposits in their liver are increasing in the United States In 2014, liver failure due to the fat deposits preventing proper functioning was the most common reason for transplantation. However, obese patients often have a challenge getting to the top of the waiting list.
Previous research has suggested that obese patients are at greater risk to undergo liver transplants. Metabolic and cardiovascular disease associated with obesity can be a major cause of death following liver transplantation. Because of this, they can be denied access to transplant services until they are below what is deemed an acceptable body mass index (BMI). For many patients though, this can be difficult to achieve and sustain, particularly for those with a medically complicated obesity.
Study examines long-term outcomes of 2006 protocol
To address the challenges in treating this group of patients, liver transplant surgeons at the Mayo Clinic in the United States developed a new protocol in 2006. If patients remained above a critical BMI at the time they were at the top of the waitlist and a liver was available for them, then the transplant would still go ahead but a weight loss surgery would be done at the same time. The weight loss surgery consisted of reducing the size of the stomach, in a procedure known as sleeve gastrectomy.
The long-term outcome from the new protocol was recently reviewed and compared with patients who had managed to lose weight pre-operatively and had undergone liver transplant alone. The findings were published in Hepatology. The researchers compared the dynamics of weight loss and gain, metabolic outcomes and quality of life between 36 patients who had liver transplant alone with eight patients who had a combined liver transplant and weight loss surgery.
Liver transplant with weight loss surgery resulted in more effective and stable weight loss after transplant
Patients who had a liver transplantation with weight loss surgery had a more profound and stable weight loss after surgery. These patients sustained a weight loss of almost 35% body weight at three years after surgery compared with only 13% in patients who did not have weight loss surgery. Measurements of metabolic status were also better in the patients who had weight loss surgery. There was no difference in the quality of life between the patients after surgery. These findings led the researchers to make several conclusions.
The combined weight loss surgery and liver transplant resulted in more effective and durable weight loss as well as fewer metabolic complications. The quality of the research does not yet lead to a straightforward recommendation for the combined surgery, however.
Researchers question the optimal timing of weight loss surgery
Researchers are left to answer whether the combined surgeries should all be performed at the same time, or whether the weight loss surgery should be done several months later. They even consider whether weight loss surgery is advantageous in patients who have managed pre-operative weight loss due to the more sustained weight loss over the ensuing years. Higher patient numbers undergoing the combined approach and further review of the results is needed before that question can be answered.
Written by Nicola Cribb, VetMB DVSc Dip.ACVS
Reference: Zamora‐Valdes D, Watt K, Kellogg T, et al. Long‐term outcomes of patients undergoing simultaneous liver transplantation and sleeve gastrectomy. Hepatology. 2018;68(2):485–495. doi:10.1002/hep.29848.